COVID-19 — WSNA advocating for you: Demanding action from top health officials and answering your questions
WSNA is continuing our advocacy at the highest state level. We shared your stories and concerns over PPE and other mixed messages on Saturday in two conference calls with officials from the Washington State Department of Health (DOH). Both Secretary of Health John Wiesman and State Health Officer Kathy Lofy spent an hour on the phone with WSNA, as well as UFCW 21 and SEIU 1199NW. We emphasized that some hospitals appear to not be following any standard protocols (CDC or WHO).
Secretary Wiesman said that Washington state has now received its first full shipment of PPE from the National Strategic Reserves. DOH is working to distribute those supplies quickly.
Staff from the Governor’s Office participated on this call, as did the Washington State Medical Association and Washington State Hospital Association (WSHA).
WSNA has been diligently cataloging the information you’ve shared with us, and on Sunday morning we sent the Governor’s Office, DOH and WSHA a document detailing some of the concerns reported by our members across the state. We will continue to demand that state leaders ensure all hospitals are keeping nurses and other health care providers safe.
WSNA believes that N-95 respirators are the gold standard and are the necessary and minimum protection for our nurses and health care workers caring for suspected and confirmed COVID-19 patients. The science of this disease is evolving. Many infectious disease experts are now reporting that due to the droplet transmission of COVID-19, surgical masks can be used.
Answering your questions
This crisis is developing very quickly, and we want to ensure you have clear, correct answers to your questions. Here are some of the top questions we are hearing and answers that include links to source information.
This article from The Seattle Times has very clear information on COVID-19 transmission and symptoms – WSNA will be sharing this on social media.
How is COVID-19 transmitted?
- Between people who are in close contact with one another (within about 6 feet).
- Through respiratory droplets produced when an infected person coughs or sneezes.
- It may be possible that a person can get COVID-19 by touching a surface or object that has the virus on it and then touching their own mouth, nose, or possibly their eyes, but this is not thought to be the main way the virus spreads.
These droplets can land in the mouths or noses of people who are nearby or possibly be inhaled into the lungs.
Source: Centers for Disease Control & Prevention
Will more testing be available?
As of March 6, 2020, the Washington State Department of Health reported that they would soon be able to run 200 tests per day. Those tests were being distributed in the order of public health importance with those living within an outbreak (e.g., Kirkland nursing care home) and health care workers being top priority.
The University of Washington is also expected to be able to run 1000 – 1,500 tests per day beginning the week of March 9, 2020.
Source: Washington State Department of Health; Washington State Epidemiologist for Communicable Disease Scott Lindquist, MD, Nursing Union TeleTownhall, March 6, 2020.
What PPE is needed when treating a COVID-19 suspected or positive patient?
Current CDC guidance for COVID 19 PPE is an N-95 respirator, gown, gloves, and eye protection. This is based on the original assumption that COVID 19 is an airborne disease process. Many infectious disease experts are now reporting that studies show COVID 19 is spread via droplet transmission; therefore, surgical masks can be used. As previously mentioned, WSNA believes that N9-5 respirators are the gold standard and are the necessary and minimum protection for our nurses and health care workers.
Source: Centers for Disease Control & Prevention
Are exposed providers supposed to rely on their employer to tell them when a patient they’ve treated tests positive?
Yes. DOH, Public Health – Seattle & King County, and other local public health officials have told us it is the obligation of hospitals to tell their employees when they have been exposed to COVID-19.
Source: Meetings with DOH, PHSKC, other LHJs via conference call.
If exposed to a COVID-19 positive patient, what are the different risk levels and what actions should be taken at each level?
On March 7, 2020, the CDC updated its guidance regarding exposure risk categories and recommendations (including work restrictions).
This updated guidance lets hospitals allow asymptomatic health care providers who have been exposed to a COVID-19 patient to continue working after options to improve staffing have been exhausted and in consultation with their occupational health program. CDC goes on to say that these health care providers should still report temperature and absence of symptoms each day prior to starting work. CDC says “[i]f HCP develop even mild symptoms consistent with COVID-19, they must cease patient care activities, don a facemask (if not already wearing), and notify their supervisor or occupational health services prior to leaving work.”
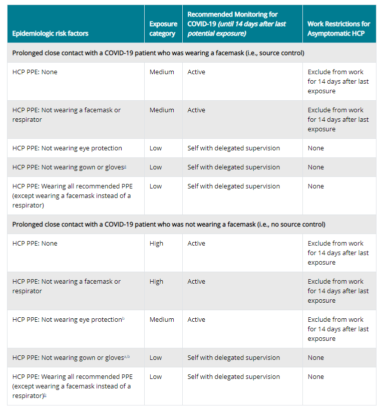
Source: Centers for Disease Control and Prevention
If I am on quarantine at home, what precautions should I take to protect my family?
Take the same steps as if you have influenza or seasonal flu.
- Call your health care provider before going in
- Stay home except to get medical care (if needed, call provider first)
- Separate yourself from other people and animals in your home
- Cover coughs and sneezes with a tissue, discard in trash, wash hands
- Wear a mask if going in car with others and in health care provider’s office
- Ensure “high-touch” surfaces are cleaned daily
Source: Centers for Disease Control and Prevention
Is there a recommendation to limit visitors during the COVID-19 outbreak?
Yes. According to DOH, visitors should be limited especially when a patient has tested positive for COVID-19.
Source: Washington State Epidemiologist for Communicable Disease Scott Lindquist, MD, Nursing Union TeleTownhall, March 6, 2020
Which countries are currently on the list for automatic quarantine if you have visited there?
As of March 8, 2020, the following countries are listed as Level 3, and non-essential travel to these countries should be avoided. Travelers from these countries should stay home for 14-days and practice social distancing upon arrival in the U.S.
- China (does not include Hong Kong, Macau, or Taiwan)
- Iran
- Italy
- South Korea
As of March 8, 2020, the following countries are listed as Level 2, experiencing sustained community transmission. Older adults and those with chronic medical conditions should consider postponing nonessential travel:
- Japan
As of March 8, 2020, the following countries are listed as Level 1, risk of limited community transmission. Travelers to these countries should practice normal precautions against illness and pay close attention to their health for 14-days after returning to the U.S.:
- Hong Kong
Source: Centers for Disease Control and Prevention
Please contact your Nurse Representative with any questions or concerns.
