Telehealth gives busy ED a partner in acute stroke care
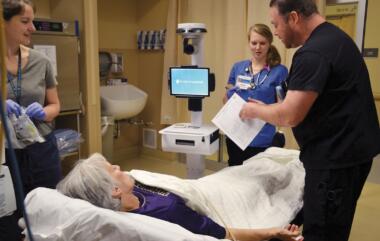
Providence Regional Medical Center in Everett is a 530-bed regional referral center with Level II trauma designation located in Snohomish County. We have a very busy Emergency Department seeing 250-275 patients per day, or approximately 90,000 patients annually. Our Code Stroke process started in 2010, and we have had more stroke alerts every year. In 2017, we activated 600 “code strokes” in ED and about 10 percent occurred in inpatient areas. Of the patients with acute stroke activations, 20 percent are cared for by Telehealth consultation. Neuro-hospitalists work 12 hours, from 7 a.m. to 7 p.m., and respond to all areas for stroke alerts. From 7 p.m. to 7 a.m., we use Telestroke with neurologists from the Swedish Medical Group Inpatient Neurology Team.
The American Stroke Association recommends that care be instituted rapidly and that protocols improve the care of stroke patients. We have stroke algorithms for the Emergency Department and Inpatient areas for both day and night shifts and treated 700 patients with a stroke in 2017.
With a Telestroke neurologist consulting via audio-video conferencing technology, the Emergency Department has a partner in the care of acute stroke patients. Via Telestroke that neurologist can examine the patient, speak to staff and family, recommend treatments, view imaging scans, write orders and assist the staff in providing care. The care that is needed quickly is lifesaving IV Alteplase and/or clot retrieval. The world of stroke care expanded in the past year with the results of two trials that showed clot retrieval can be done in carefully selected stroke patients in a greatly expanded timeframe, which is up to 24 hours after symptom onset.
For the RN, the skills involved with Telestroke are very similar to when neurology is on-site. However, Telestroke requires certain technical and troubleshooting skills. For the patient to receive the best care, the monitor setup must be optimal. RN education is provided in the use of the technology and assisting the provider with remote neuro exams.
It is also very important to be well versed in the NIH Stroke Scale. One must be very comfortable with the NIHSS and do it well in order to best assist the remote neurologist in their examination of the patient. A critical care RN responds to each code stroke and this RN usually performs the NIHSS scoring. In the interest of time, the Telestroke patients have a completed computerized tomography (CT) scan prior to the neurologist’s examination. During the day, on-site neurologists triage some code strokes. ED will always defer to their judgment. With code strokes at night, we utilize the on-call Telestroke neurologist and run a code stroke over the Telestroke cart. Nurses need to rely on their strong neuro assessment skills and be comfortable with patient advocacy to be effective in the Telestroke environment.
The following vignette, told by Mary Linares, ED RN, demonstrates the high quality, expert care that the team is able to deliver quickly with the help of Telestroke:
ED receives a medic call of a possible code stroke. EMS reports new dysarthria, aphasia, dizziness, vomiting and ataxia. Patient’s last seen normal was tonight at 23:00. An internal ED Code Stroke is called. Patient arrives at 23:20. The medics with the patient are met in the stroke alcove, right at the ambulance bay doors. Here, an ED MD quickly evaluates the patient’s deficits, history and risk factors. Simultaneously, the ED RNs enter stroke orders, obtain venous access and draw labs, which are handed over to the ED lab tech for immediate processing. These labs include an iStat creatinine, which takes just a few minutes to result. The ED MD decides to proceed with the code stroke. The patient is stable and so proceeds directly to CT with two RNs via the EMS gurney. This entire process takes less than five minutes.
While the patient is on the CT table receiving their non-contrast head CT, the lab calls to report that the creatinine is WNL, so a CT Angiogram head is also ordered and performed immediately after the non-contrast study. During this time, the ED pharmacist is checking in with the team to discuss the likelihood of giving TPA. At the same time, the ED technician is setting up the Telestroke monitor in the patient’s room.
When the imaging is complete and the patient moves to their ED room, the ED MD is already there and the Telestroke monitor is set up so that the remote neurologist has the fullest view possible of the patient’s bed. The ED MD and the neurologist have already spoken by phone. Now the neurologist performs a full NIHSS of this patient, with assistance from the on-site staff. The NIHSS is 6. There are no contraindications to TPA, so it is ordered. Pharmacy delivers the bolus and infusion within 10 minutes, and the TPA is started. The patient’s time in ED is just 49 minutes.
Meanwhile, the CTA head shows a retrievable clot. This same neurologist seeing the patient via Telestroke viewed scans and recommends clot retrieval. Serial NIHSS scores improve from 6 to 4 prior to clot retrieval.
Telestroke providers working with on-site providers and nurses complete a team that provides high quality, expert stroke care no matter what time of day or night an emergency occurs. Our staff are familiar with stroke symptoms are able to call for consultation, making Telestroke very valuable for patient care.
