Long-term care in Washington

This content originally appeared in the Spring/Summer 2020 issue (PDF) of The Washington Nurse magazine. See the full set of stories on long-term care.
Long-term care covers many different care settings, including skilled nursing, assisted living facilities and adult family homes. It is a sector that continues to grow as people look for community-based options that meet their medical care and assisted living needs. And the need for long-term care is only expected to grow. The U.S. Congressional Budget Office estimates that by 2050, one-fifth of the total U.S. population will be 65 or older, up from 12% in 2000 and 8% in 1950.
As of January 2020, the Washington State Department of Social and Health Services’ roster of licensed communities included 209 skilled nursing facilities, 540 assisted living facilities and 3,135 adult family homes. Together, they serve more than 67,000 people.
Without skilled, professional nurses, alternative care community options would not be successful.
In 2018, the Washington Center for Nursing and the University of Washington Center for Health Workforce Studies conducted a survey with the goal of identifying practice areas and RN attitudes. The report focused on the approximately 63,122 RNs who were actively employed and practiced in Washington state. They found that nearly 12% worked in long-term care, which included assisted living facilities, home health, hospice and nursing home/extended care.
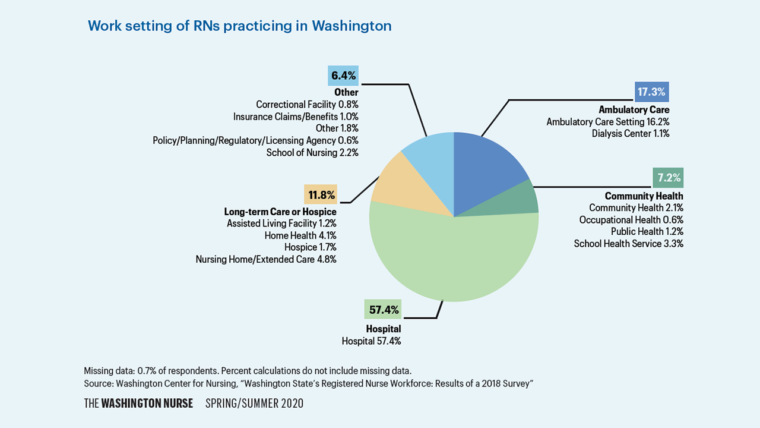
Skilled nursing
Most residents living in skilled nursing communities require direct nursing supervision because of complex health care related to multiple medical issues. In addition, according to the National Center for Health Statistics, 47.8% of nursing home residents were diagnosed with Alzheimer’s disease or other dementia. Skilled nursing care is highly regulated, and nurses must assure that licensing requirements are met. The nurse’s role includes extensive multi-system assessments and documentation of medical and social, memory loss and mental health behavior as well as skin health and falls. RNs oversee care staff and coordinate with health care providers, discharge planners/case managers and community partners. Resident needs may include wound care, IVs, injections, rehab, dialysis and hospice care. Nurses also oversee infection control, care staff CE and immunizations. Nurses must be present 24 hours a day.
Assisted living communities
Today, most assisted living communities offer an extensive menu of personal care services as well as health management. Communities devoted to seniors with memory loss are common throughout the state. Registered nurses and LPNs are now necessary to oversee services to assure the safety and appropriate care of community residents, and assisted living regulations have become complex. As the primary medical staff, nurses need comprehensive assessment skills and a current medical knowledge base in order coordinate complex resident medical needs. Nurses interact daily with community providers, health care providers, discharge planners/case managers and community partners. They coordinate with hospital case managers and discharge planners; individual resident health care providers; and home health, hospice and palliative care workers to allow residents to stay in their familiar surroundings with support.
Adult family homes
Adult family homes are licensed for up to six persons. The number of homes has grown substantially since 1995. A nurse may own one or several adult family homes and therefore can coordinate care similar to assisted living nurses although the majority of these homes do not have a licensed person who owns them or is the manager of record. With up to six residents, adult family home care can be more individualized, especially for residents with memory loss. Residents have the same complex health care issues as with other community settings.
Registered nurse delegators are an integral part of this system, and practice is regulated under Washington State law. The RN delegator visits the home frequently to assess residents for any medical changes and train caregivers to provide for those care needs within their licensure. The RN delegator constantly updates assessments and individual care plans as health care needs evolve.
Home care
Home care agencies employ RNs for hourly care, either paid privately or by insurance. Skilled home health services include wound care, patient and caregiver education, intravenous or nutrition therapy, administration of injections and monitoring serious illness and unstable health status. One such agency provides hourly care to pediatric populations who are on ventilators or have multiple complex care needs requiring almost hourly supervision to prevent complications and ongoing family or caregiver training.
WSNA Community-Based and Long-term Care Nurse Practice Task Force
This specialty task force was approved by the WSNA Board of Directors in 2018 to shine a light on the work being done by our registered nurse colleagues in this growing sector. Goals for the task force include the following:
Identify and address issues of importance to nurses working in long-term care settings.
Increase awareness within WSNA and the broader nursing community about the opportunities of working in long-term care as a viable employment opportunity.
Strengthen the transitional care processes between acute care settings and LTC community-based settings, considering the respective roles and responsibilities of acute care and LTC nurses.
Work with the Washington State schools of nursing to better integrate LTC/skilled nursing care practice into the curriculum.
Current task force members represent education, management, LTC practice, ER nursing and policy. To draw in a broad spectrum of views and experience, task force members are not required to be WSNA members.
Would you like to be a part of this work?
WSNA is seeking additional members of the Community-Based and Long-Term Care Task Force. To express your interest, email Sally Watkins at swatkins@wsna.org.
